|
3/1/2024 0 Comments Mog antibody testing order
This assay was developed using the MOG construct provided by Dr Waters,(11) and the validation was based on a blinded comparison with the Oxford assay. This study provides Class II evidence that the presence of serum MOG-IgG1 distinguishes non-MS CNS demyelinating disorders from MS (sensitivity 24%, 95% CI 9%-45% specificity 100%, 95% CI 88%-100%). 
All 7 patients with probable MS were MOG-IgG1 negative. The clinical diagnoses obtained in 33 MOG-IgG1-positive patients included 4 NMO, 1 ADEM, and 11 optic neuritis (n = 11). Testing of 1109 consecutive sera sent for AQP4-IgG testing(12) revealed 40 AQP4-IgG and 65 MOG-IgG1-positive cases. MOG-IgG1 was detected by cell-based assay in 8 (38%) of these cases.(13) Of 58 patients fulfilling 2006 Wingerchuk criteria for NMO, 21 (36%) tested negative for AQP4-IgG. Using a similar assay to this MOG-IgG1 flow cytometry assay, demonstrated high specificity of their MOG-IgG1 assay in which 49 patients with MS, 13 healthy control sera, and 37 AQP4-seropositive serum samples were all negative at a dilution of 1:20. The detection of MOG-IgG1 allowed non-MS demyelinating diseases (ADEM, AQp4-IgG negative neuromyelitis optica spectrum disorder including ON,TM) to be distinguished from MS.(12) They showed that their MOG-IgG1 flow cytometry assay eliminated false positive results without losing true positive results with low titers. In 2015, Waters and colleagues (11) from Oxford University established a novel cell-based assay for the measurement of IgG1 MOG antibodies based on previous findings that MOG antibodies are almost exclusively of the IgG1 subclass. Therefore, early diagnosis and initiation of appropriate immunosuppressant treatment is important to optimize the clinical outcome by preventing further attacks. 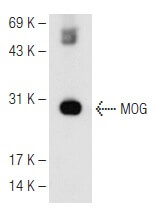
Disease-modifying agents, treatments promoted for MS, have been reported to exacerbate MOG-IgG1 seropositive IDDs. Detection of MOG-IgG is diagnostic of central nervous system (CNS) inflammatory demyelination, where the clinical phenotype (NMOSD, optic neuritis, transverse myelitis, ADEM) may be similar, but the immunopathology (astrocytopathy vs oligodendrogyopathy) and clinical outcome (worse vs better) are different.(9) Detection of MOG-IgG also predicts relapse.(10) More importantly, MOG-IgG seropositive IDDs are distinct from MS and treated differently.(8, 9) Treatments for IDDs seropositive for MOG-IgG include corticosteroids and plasmapheresis for acute attacks and mycophenolate mofetil, azathioprine, and rituximab for relapse prevention. More effective treatments combined with earlier and more accurate diagnosis has led to improved outcomes.Īpproximately 80% of patients with NMO are seropositive for aquaporin-4 (AQP4)-IgG.(5-7) In the remaining 20% of patients, myelin oligodendrocyte glycoprotein (MOG)-IgG is detected in up to a third.(8) The pathogenic target for the remaining patients remains unknown. Many patients with NMOSD are misdiagnosed as having MS. 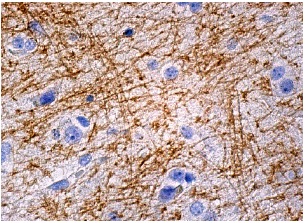
Some patients may present with acute disseminated encephalomyelitis (ADEM). Neuromyelitis optica (NMO), sometimes called Devic disease or opticospinal multiple sclerosis (MS) is a severe, relapsing, autoimmune, inflammatory and demyelinating central nervous system disease (IDD) that predominantly affects optic nerves and spinal cord.(1) The disorder is now recognized as a spectrum of autoimmunity (termed NMO spectrum disorders: NMOSD).(1-3) Brain lesions are observed in more than 60% of patients with NMOSD and approximately 10% will be MS-like.(4) Children tend to have greater brain involvement than adults, and brain lesions are more symptomatic than is typical for adult patients.(3) The clinical course is characterized by relapses of optic neuritis or transverse myelitis or both.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
